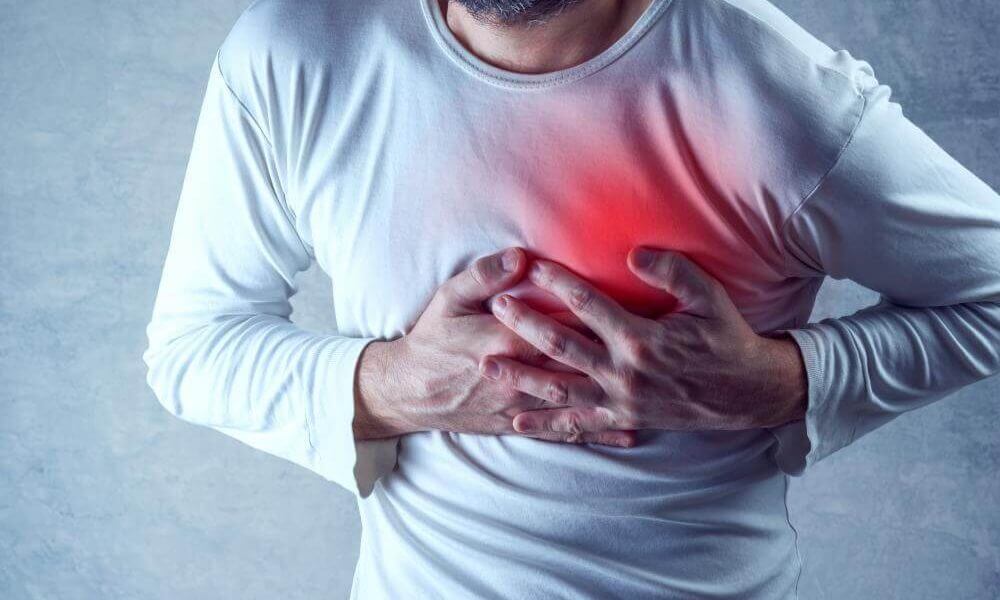
Cigna Drops OxyContin Coverage To Slow Down The Opioid Epidemic
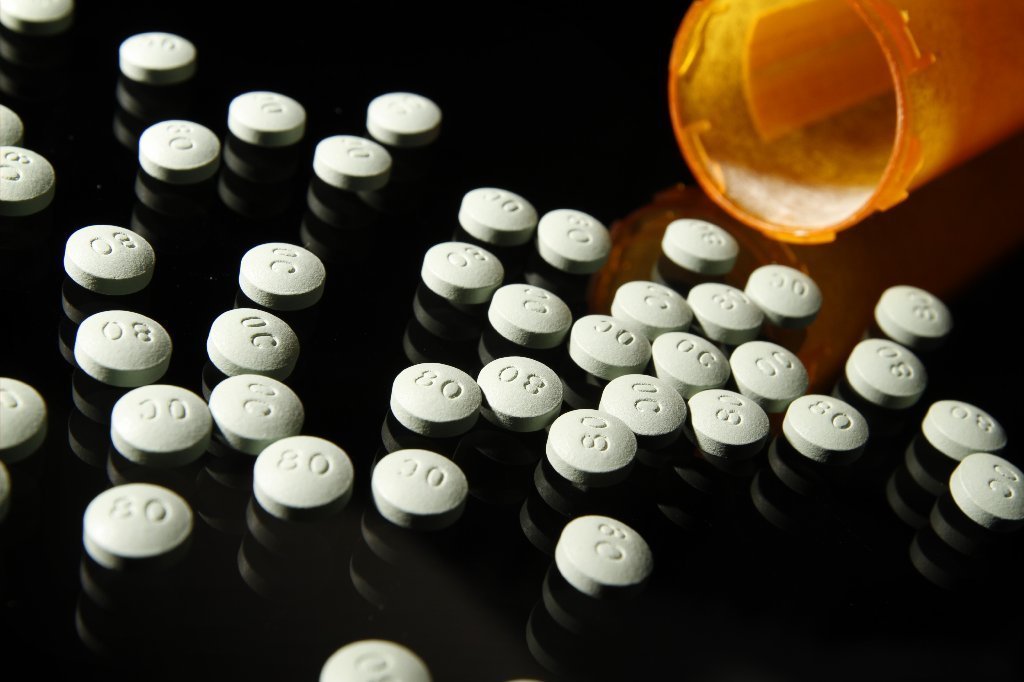
A top medical health insurance corporation is joining the combat towards the opioid epidemic.
Cigna says it might not cover prescriptions for the brand OxyContin for most customers beginning next year — it will be taken off group preferred commercial drug lists.
In 2016, Cigna laid out a 3-year plan to reduce down on opioid use among its clients by a quarter. It seems this move is an attempt to assist meet that goal.
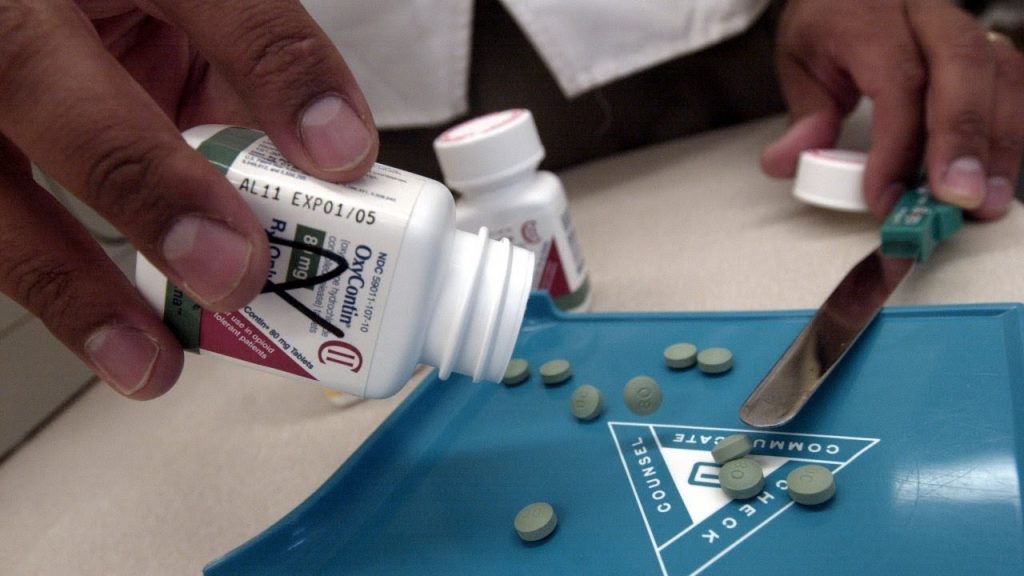
There are some caveats to this announcement: Cigna will still cover at least one oxycodone alternate, and those who use OxyContin for hospice or cancer care could have their prescriptions covered. The corporation also says it will take into account approving OxyContin if a client’s doctor deems it medically necessary.
Cigna is informing patients with current OxyContin prescriptions and their doctors about the future change.
“while drug companies do not manipulate prescriptions, they can help influence patient and doctor conversations via educating people about their medications. The insights we achieve from the metrics in the new value-based contract will help us continue to evolve our opioid management strategies to help our customers and their doctors,” Jon Maesner, Cigna’s chief pharmacy officer, said.
The latest statistics from the Centers for Disease Control and Prevention show that 33,000 people had been killed by opioid overdoses in 2015, and nearly half of those overdose deaths involved a prescription opioid.