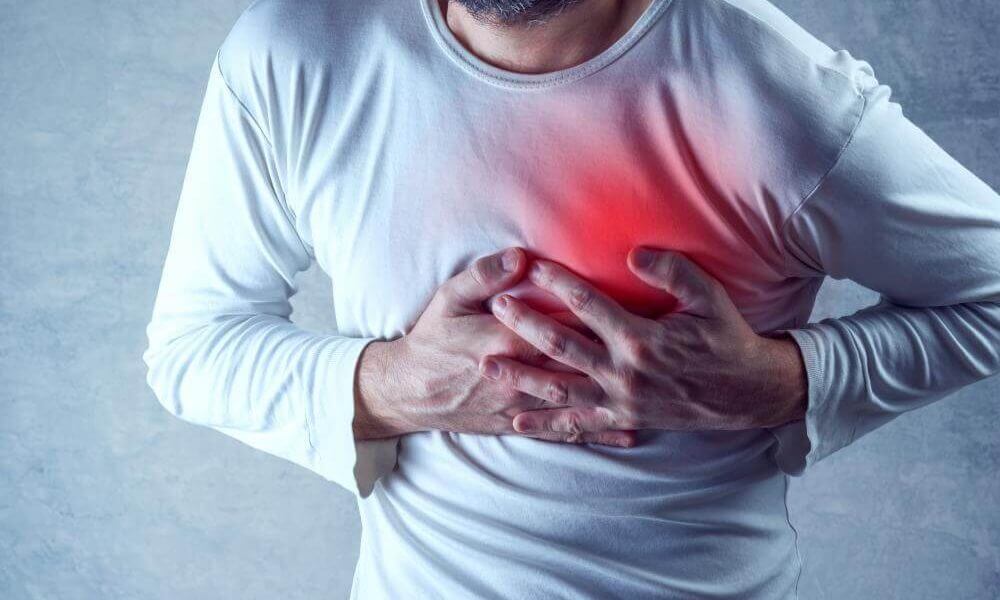
What Is The Acute Myocardial Infarction
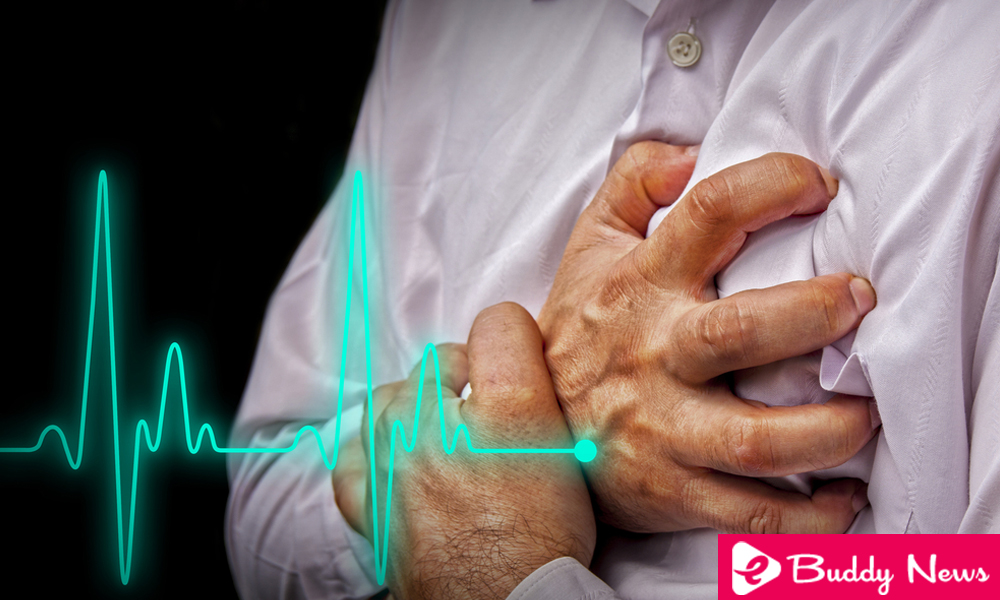
Acute myocardial infarction is a medical emergency, of extreme severity, due to its high mortality rate. In addition, it is one of the main causes of death in our environment together with cancer.
Generally, the death of muscle fibers in the heart is called “acute myocardial infarction”.
Based on the findings that appear on the electrocardiogram, heart attacks can be classified as:
- Acute myocardial infarction with ST-segment elevation.
- Acute myocardial infarction without ST-segment elevation.
This classification is very useful since it determines the initial therapeutic attitude that the patient must receive from the medical staff.
Epidemiology of acute myocardial infarction
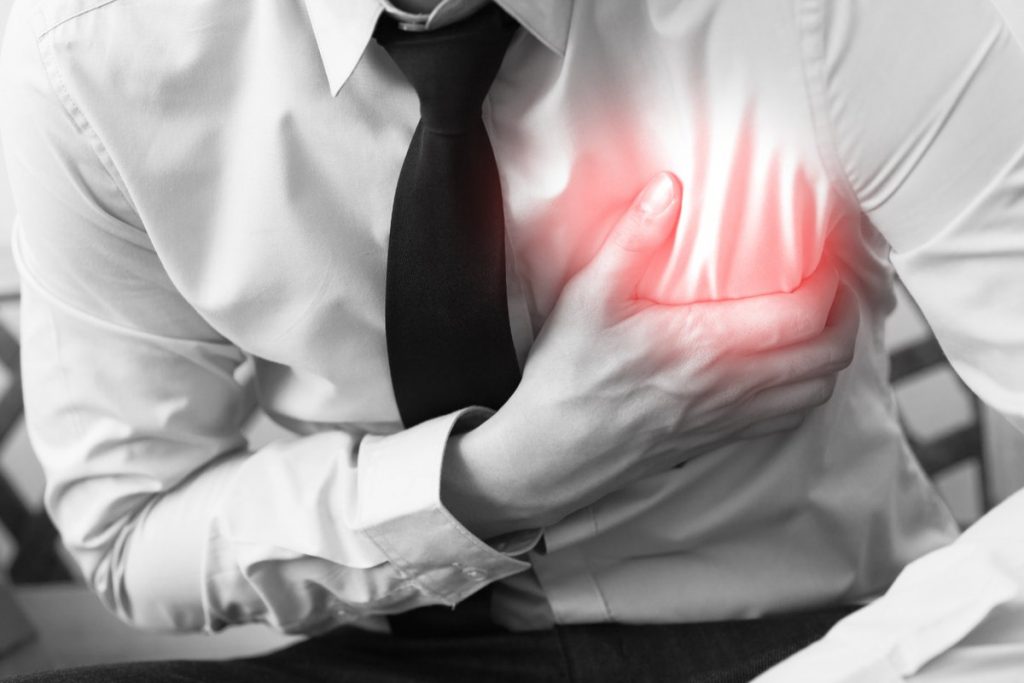
Myocardial infarction is the cause of around 13 million deaths per year.
It is slightly more common in men than in women. It is estimated that in Europe 1/6 men, compared to 1/7 women will die from a myocardial infarction.
Risk factor’s
There are a number of factors that increase the risk of heart attack, some of them correctable, such as toxic habits. The most relevant are:
- Age> to 65 years.
- Male sex
- Diabetes mellitus.
- Arterial hypertension.
- High cholesterol.
- Obesity, smoking, drug use, sedentary lifestyle, among others.
- Presence of other cardiac pathologies.
How is a heart attack?
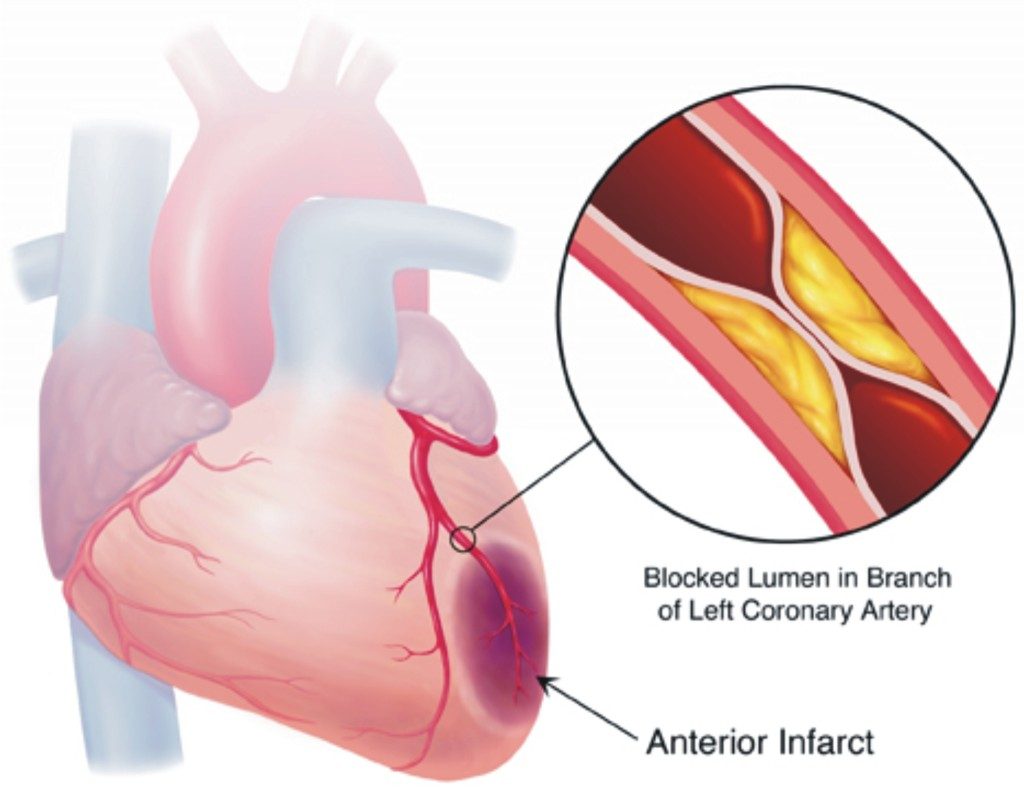
The most common cause is the occlusion of the coronary arteries, the arteries that supply the heart, with a thrombus. It comes, in most cases, from a plaque of fat that accumulates in the arteries.
When the fatty plaque (atheroma) breaks, a piece is detached, and this will travel through the circulation of blood. And finally it will reach the coronary arteries, there it will occlude them. D this way, the heart runs out of blood flow.
Although it is rarer, in some cases the thrombus can be produced by an excess of blood coagulation. Other rare causes are aortic dissection, congenital anomalies, trauma, congenital anomalies, among others.
What tells us that a heart attack is occurring?
The symptoms of a heart attack are well known to everyone. Even so, to determine with certainty that a heart attack exists, a series of clinical requirements must be met. These requirements are:
- Symptoms of infarction.
- Evidence in the electrocardiogram.
- Finding a thrombus in the coronary arteries.
- Evidence of cardiac damage in biochemical tests.
What are the symptoms and signs of myocardial infarction?
- Thoracic pain. It is sudden and prolonged (more than 30 minutes normally). It is perceived in the center of the chest, as a weight or very intense pressure. It usually extends to the left arm and shoulder, including the neck and jaw.
- Very abundant sweat.
- Nausea and vomiting.
- Pallor.
- The sensation of breathlessness, difficulty in breathing.
- Anguish feeling.
- The external appearance of extreme gravity.
Atypical presentations:
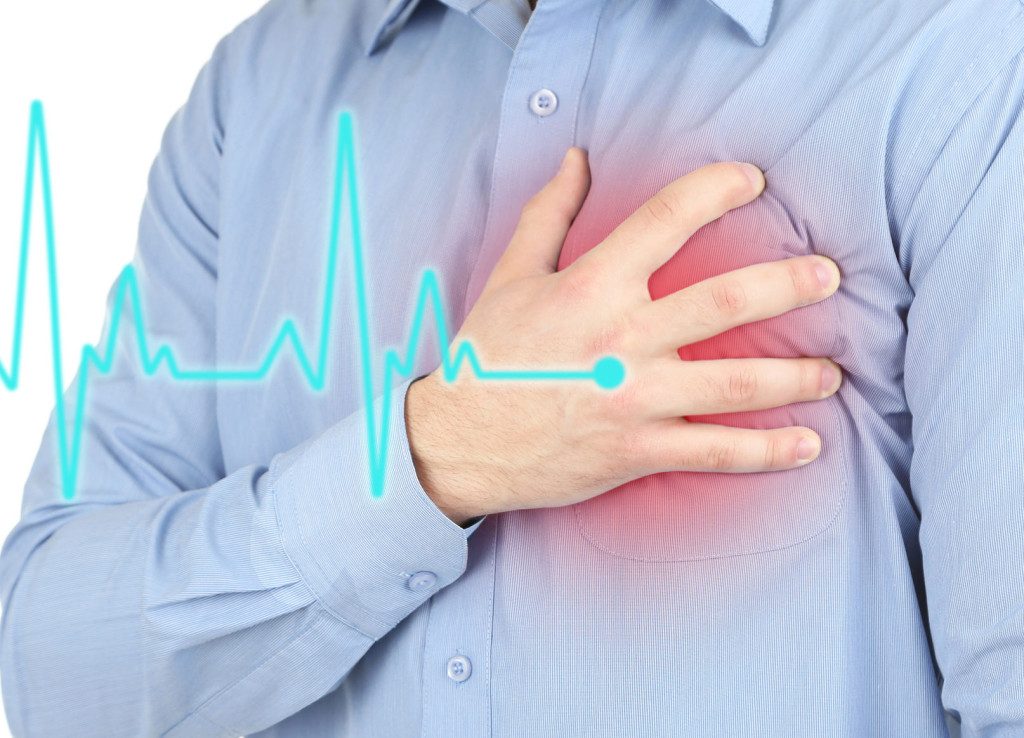
A heart attack does not always present as chest pain. Although the typical presentation of the infarction is the most common, on some occasions, especially in the elderly and diabetics, the clinical picture that appears is different.
- Myocardial infarction without pain (30%). He has the extreme and inexplicable weakness, sweating, nausea and vomiting, paleness, respiratory distress … but there is no pain.
- Infarction with pain, but with atypical characteristics. Some patients feel pain in the abdomen, in the neck and jaw … In fact, although it is relatively rare, in the presence of a patient with acute abdomen, an electrocardiogram is required.
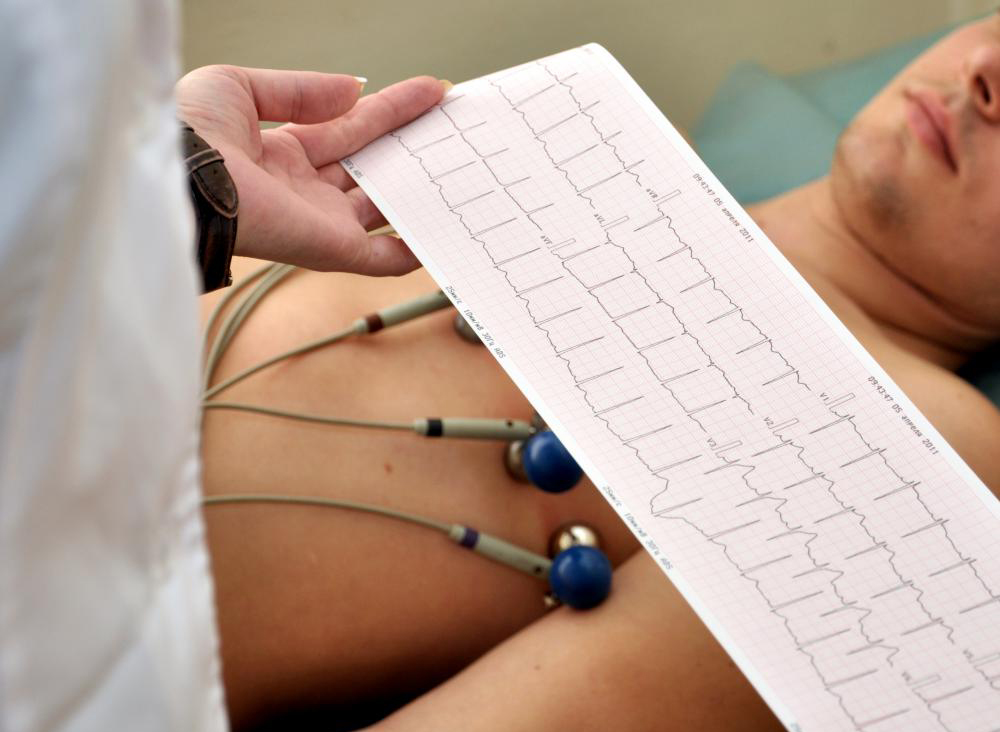
What do we find in an electrocardiogram of a person who is suffering a heart attack?
The alterations of the electrocardiogram depend on the moment in which it is performed. That is to say, as the infarction evolves, the path changes.
Even so, the most characteristic elements are:
- Alteration of T waves, which become very pointed and high. Indicates subendocardial ischemia.
- In the case of infarction with an elevation of the ST segment, it rises more than 1 mm in more than two leads. In the infarction without elevation of the ST segment, the rest of the pathological findings appear.
- It is possible to find Q waves, which indicate necrosis.
What are biochemical markers? How can they be used to diagnose a heart attack?
Biochemical markers are a series of molecules that can be detected in the blood by analyzing them. Their concentrations increase or decrease gradually in certain situations, which is used for diagnostic purposes.
In the case of myocardial infarction, the markers used are proteins that the muscle fibers release when they die. These proteins are:
- Myoglobin
- The CPK-MB.
- The troponins.
Troponins are the only ones that are released exclusively in the cells of the heart. The other two proteins are released by both cardiac cells and the rest of the fibers of other muscles. That is the reason why troponins are the most specific markers for the diagnosis of cardiac infarction.
How is it diagnosed?
- Very detailed clinical history and complete physical examination.
- Along with the medical history, it is the most valuable tool. In the presence of a patient who may be suffering from a heart attack, the ECG should not be delayed.
- Biochemical analysis
- Imaging techniques, both invasive and non-invasive.
Cardiac ultrasound is the most valuable technique, as it is non-invasive and, in addition, relatively fast. Regarding invasive tests, the technique that offers the best results is coronary angiofraphy (coronariography).
Treatment of acute myocardial infarction
The objectives of the treatment are the reduction of the infarct size and the early diagnosis and treatment of possible complications.
The treatment of acute myocardial infarction must be immediate. 30% of patients die within the first hour, the most frequent cause being ventricular fibrillation.
Immediate care
- Monitoring of vital signs: heart and respiratory rate, oxygen saturation and blood pressure.
- Rest and fluid administration.
- Oxygen in nasal glasses if the saturation is below 95%
- Treatment of pain and anxiety with opiates (morphic chloride) and anxiolytics. Anxiety and pain increase the work of the heart, which can ultimately cause the size of the infarct to increase.
- Antiaggregants: acetylsalicylic acid (250mg) with P2Y12 inhibitor.
- Beta-blockers to control blood pressure.
- Atropine to control the heart rate.
Reperfusion treatment
It is based on the recanalization of the occluded artery and its benefit is maximum in the first 12 hours. There are two ways to do it:
- Using fibrinolytic drugs. They are indicated when angioplasty is not possible within the first 2 hours after diagnosis. After administering the drugs, the patient should be referred to a center trained to perform the angioplasty.
- Urgent angioplasty. It is the technique of choice if it can be done within the first two hours from the medical contact.